Translate this page into:
Genetic susceptibility to Tuberculosis in an infant with BCG-osis
*Corresponding author: Mukesh Desai, Department of Immunology, Bai Jerbai Wadia Hospital for Children, Mumbai, Maharashtra, India. desai.mm18007@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Manwar MS, Gowri V, Taur P, Iyengar V, Chougule AS, Desai M. Genetic susceptibility to Tuberculosis in an infant with BCG-osis. Wadia J Women Child Health. 2023;2(3):136-9. doi: 10.25259/WJWCH_24_2023
Abstract
Mendelian susceptibility to mycobacterial diseases (MSMD) is a group of innate immunity defects characterized by inborn susceptibility to intracellular pathogens. These are due to defects in the interleukin 12-23-interferon gamma y axis. Twenty-three genetic mutations have been identified in this axis, of which mutation in the IL12RB1 gene is the most common genetic defect of MSMD identified. An 11-month-old infant presented with features of axillary lymphadenitis and skin lesions both of which were positive for acid-fast bacilli on Ziehl– Neelsen stain and GeneXpert. Keeping a high index of suspicion of primary immunodeficiency, the child was evaluated further and was diagnosed as a case of MSMD with IL12RB1 gene mutation.
Keywords
Bacillus Calmette Guerin
Genetic susceptibilty to tuberculosis
Interferon gamma
Mendelian susceptibility to mycobacterial diseases
INTRODUCTION
Mendelian susceptibility to mycobacterial diseases (MSMD) is a group of innate immune defects localized to 23 genes and 37 clinical phenotypes. Interleukin (IL)-12/23/interferon-stimulated gene 15 (ISG15)-interferon gamma (IFN-γ) axis is the principal immunological pathway for intra-macrophagic pathogens. Defects in this pathway lead to an inborn susceptibility to intracellular pathogens such as Mycobacteria (including Bacillus Calmette Guerin (BCG) vaccine strains and Non Tuberculous Mycobacteria), Salmonella, Fungi (Candida, Histoplasma), parasites like Leishmania, and some viruses like Cytomegalovirus (CMV). Mutations in the IL12RB1 gene are the most common genetic defect identified in MSMD.
CASE REPORT
An 11-month-old male infant, first born of the non-consanguineous union, with normal birth, developmentally normal, and completely immunized, was referred to our institute with a swelling at the BCG injection site since 5 months of age. At 10.5 months of age, he developed a painful swelling in the left axilla with fever, which later developed into an abscess. There was history of tuberculosis in the mother at 8 years of age and in the father at 10 years of age; however, no microbiological confirmation was available for the same. No history of early-onset tuberculosis (TB) in other extended family members was present.
On examination, he was well-grown with length (75 cm), weight (9.5 kg), and head circumference (45 cm) between −1 standard deviation to the median. On local examination, the left deltoid had a non- tender erythematous papule with no discharge [Figure 1]. The left axillary node was enlarged (2×2.5 cm), fluctuant and tender [Figure 2]. Systemic examination was otherwise unremarkable.

- Erythematosus indurated non-tender papule.

- Left axillary node, fluctuant and tender 2*2.5 cm in dimensions.
Chest X-ray was normal. Ultrasonography (USG) of the left axilla showed 4 to 5 lymph nodes with abscess formation. Incision and drainage of the abscess was done and pus was Ziehl Neelsen stain and GeneXpert, positive. Pus culture isolated the MTB complex. The child was started on isoniazid, rifampicin, pyrazinamide (PZA), and ethambutol, as per Revised National Tuberculosis Control Program (RNTCP) protocol.
On follow-up 15 days later, the left axillary node continued to drain pus and there were new-onset skin lesions papulomacular in nature with central crusting [Figure 3]. Punch biopsy of the skin lesion was also found to be acid-fast bacilli and GeneXpert positive. As two sites i.e., axillary nodes and skin were involved a diagnosis of BCG-osis was made and an attempt was made to look for dissemination. USG abdomen, repeat chest X-ray, and gastric lavage GeneXpert performed was normal. Meanwhile, drug sensitivity revealed PZA resistance confirming disseminated Mycobacterium bovis infection [Figure 4]. On Isoniazid, Rifampcin, Ethambutol (HRE)+Ofloxacin there was good clinical response.

- Skin lesions papulo-macular with central crusting.
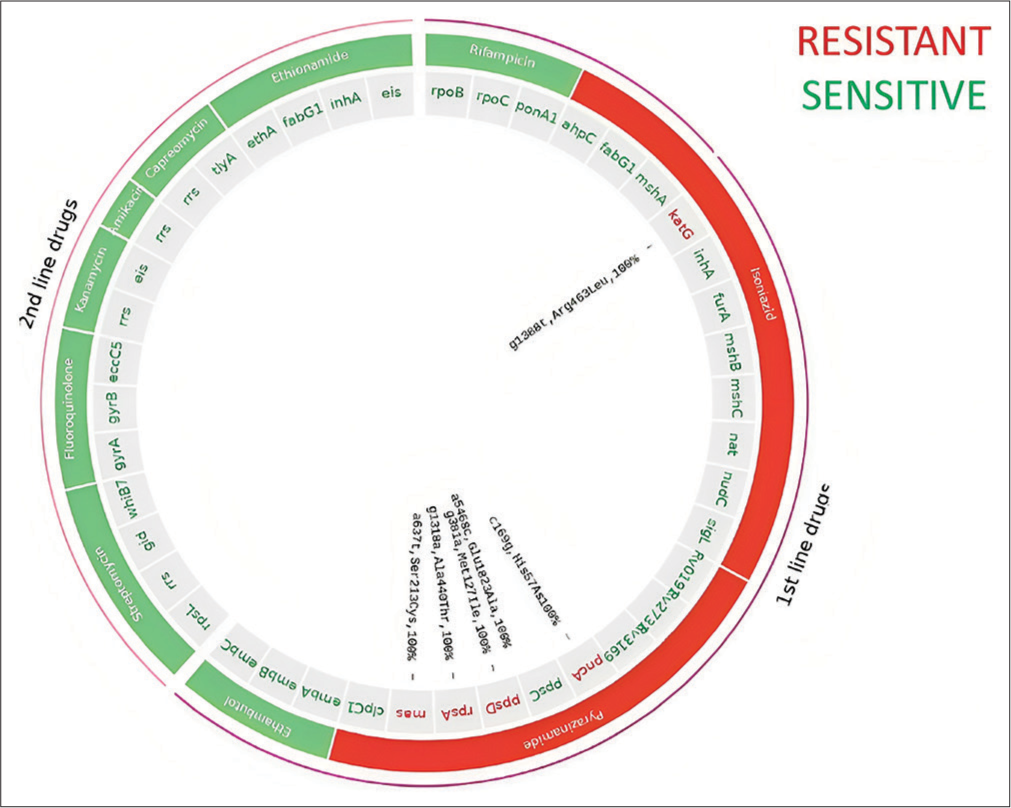
- Genome sequencing of mycobacterial tuberculosis complex from culture showed 95.2% of the markers for the lineage tool mapped to Mycobacterium bovis.
As BCG-osis can be a presenting feature of the phagocytic defect chronic granulomatous disease (CGD) and defects in innate immunity (MSMD), primary immunodeficiency was suspected and an immunological workup was done. Lymphocyte subset assay and immunoglobulin levels were normal. CGD was ruled out as the nitroblue tetrazolium test and dihydrorhodamine test were normal. MSMD was suspected in view of BCG-osis. Flow-cytometric expression of CD212 (IL12RB1) on activated T cells was 27% against the control of 75%. Hence, Whole Exome Sequencing was done to identify the genetic defect driving MSMD, which identified a homozygous deletion in the IL12RB1 gene.
DISCUSSION
MSMD is a rare condition secondary to mutations in at least one of the genes encoding cytokines, receptors, and/or their relative essential modulators of the IL12/23-IFN-γ axis.[1] If this pathway is defective, the individual becomes more vulnerable to intracellular pathogens such as mycobacteria, including attenuated M. bovis-BCG vaccine strains, non-tuberculous environmental mycobacteria, salmonella, fungi, parasites like Leishmania, and some viruses like CMV. The identified mutations were reported to be in IFNGR1, IFNGR2, IL12B, IL12Rˇ1, signal transducer and activator of transcription 1 (STAT1), IKBKG, CYBB, RORc, IRF8, ISG15, TYK2, JAK1, and NEMO resulting in impaired cellular responses and susceptibility to mycobacterial infections.[2]
Mutations in IL12RB1 (with 191 variants reported in 17 exons) are the most affected gene among MSMD patients.[3] IL12RB1 deficiency results in the absence of a functioning receptor for both IL12 and IL23 cytokines.[4] The production of IFN-γ by T cells and NK cells in response to intracellular infections is greatly aided by IL12.[5] IL23 is a key mediator in employing different components of innate immunity through the induction of IL17 production. IL17 stimulates the production of pro-inflammatory cytokines, chemokines, and prostaglandins.[6] Therefore, any IL-12 receptor dysfunction may be associated with a greater propensity to become infected with non-typhoidal Salmonellae, poorly pathogenic Non-Tuberculous Mycobacterial infections, and fungal infections.[7] Therefore, patients with IL12RB1 mutation along with susceptibility to Mycobacteria are also known to have reported infections with Candida, Histoplasma, Giardia, Staphylococcus, Proteus, Enterococcus, and Clostridium difficile. Defects in the TH17 pathway caused by IL12RB1 are also linked to autoimmunity and autoinflammatory disease. Autoimmune manifestations in the form of inflammatory bowel disease and autoimmune hemolytic anemia with leukocytoclastic vasculitis have been reported.[8] IL-12 signaling pathway also regulates Fas ligand expression, defect of this regulation in patients with IL12RB1 mutations may be a potential cause of presentation with autoimmune lymphoproliferative syndrome-like disease.[9] These unusual presentations with autoimmunity are not reported in the world literature and need further evaluation.
Different mutations cause heterogeneity in the clinical manifestations and prognosis of the disease. MSMD increases the risk of infection by a particular intracellular pathogens. About 4–80% of MSMD patients may present with BCG-related problems (the practice of immunizing all newborns shortly after delivery may be the cause of this). According to the largest cohort study of MSMD patients conducted in India,[8] the most common clinical presentation was disseminated BCGosis (82% of patients). Furthermore, all patients in the cohort had Mycobacterial disease with MTB complex (96%), and nontuberculous mycobacteria in (4%). Multisystem involvement with Mycobacteria was the most common followed by lymph node involvement, tubercular osteomyelitis, pulmonary, skin, and central nervous system. Moreover, around one-third of patients were infected with more than one organism.
Cytokine production assay, flow cytometry-based tests targeting surface receptors/cytokines/phosphorylated STAT molecules, molecular detection, and other tests are widely used for the evaluation of MSMD.
Treatment options constitute antitubercular treatment (ATT) modified on the basis of drug sensitivity usually given for the duration of 6 months to 2 years based on the site of involvement. ATT may have to be continued for longer periods possibly even for life, and other anti-infective and anti-viral drugs can be selected according to the type of infection. IFN-γ therapy is also available. Hematopoietic stem cell transplant is the definitive treatment. Our patient was continued on ATT for a period of 18 months and currently is on regular follow-up and is clinically well.
CONCLUSION
A high index of suspicion for MSMD should be kept in patients presenting with adverse effects of BCG vaccination and should be investigated for the same.
Ethical approval
Institutional Review Board approval is not required.
Declaration of patient consent
Patient’s consent not required as patients identity is not disclosed or compromised.
Conflicts of interest
There are no conflicts of interest.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The authors confirm that there was no use of artificial intelligence (AI)-assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
Financial support and sponsorship
Nil.
References
- Non-tuberculous mycobacterial cervical lymphadenitis in the immunocompetent child: Diagnostic and treatment approach. Expert Rev Anti Infect Ther. 2014;12:959-65.
- [CrossRef] [PubMed] [Google Scholar]
- Mendelian susceptibility to mycobacterial disease: Genetic, immunological, and clinical features of inborn errors of IFN-γ immunity. Semin Immunol. 2014;26:454-70.
- [CrossRef] [PubMed] [Google Scholar]
- A role for interleukin-12/23 in the maturation of human natural killer and CD56+ T cells in vivo. Blood. 2008;111:5008-16.
- [CrossRef] [PubMed] [Google Scholar]
- Interferon-gamma and interleukin-12 pathway defects and human disease. Cytokine Growth Factor Rev. 2000;11:321-33.
- [CrossRef] [PubMed] [Google Scholar]
- Role of interleukin-12 family cytokines in the cellular response to mycobacterial disease. Int J Infect Dis. 2010;14:e366-71.
- [CrossRef] [PubMed] [Google Scholar]
- The IL-23-IL-17 immune axis: From mechanisms to therapeutic testing. Nat Rev Immunol. 2014;14:585-600.
- [CrossRef] [PubMed] [Google Scholar]
- IL-23/IL-17A Dysfunction phenotypes Inform possible clinical effects from anti-IL-17A therapies. J Invest Dermatol. 2015;135:1946-53.
- [CrossRef] [PubMed] [Google Scholar]
- Clinical and molecular findings in Mendelian susceptibility to mycobacterial diseases: Experience from India. Front Immunol. 2021;12:631298.
- [CrossRef] [PubMed] [Google Scholar]
- Deregulation of Fas ligand expression as a novel cause of autoimmune lymphoproliferative syndrome-like disease. Haematologica. 2015;100:1189-98.
- [CrossRef] [PubMed] [Google Scholar]






