Translate this page into:
Manual pre-pubic compression test: A bedside examination tool in babies with atypical genitalia
*Corresponding author: R. R. Prashanth, Department of Neonatology, Seth GS Medical College and King Edward Memorial (KEM) Hospital, Mumbai, Maharashtra, India. prash2635@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Tehsin P, Prashanth RR, Nair S, Haribalakrishna A. Manual pre-pubic compression test: A bedside examination tool in babies with atypical genitalia. Wadia J Women Child Health. 2023;2(3):146-7. doi: 10.25259/WJWCH_42_2023
A 2,800-gram baby was born to a multigravida mother at term gestation through cesarean section. The baby was referred to our center as a suspected case of disorder of sexual differentiation (DSD). The neonate was noted to have an absent phallus with bilateral scrotal sacs with well-formed rugae with descended left testis and the right testis in the inguinal region [Figure 1]. The rest of the physical examination was unremarkable. The neonate was hemodynamically stable and was on exclusive breastfeeds.
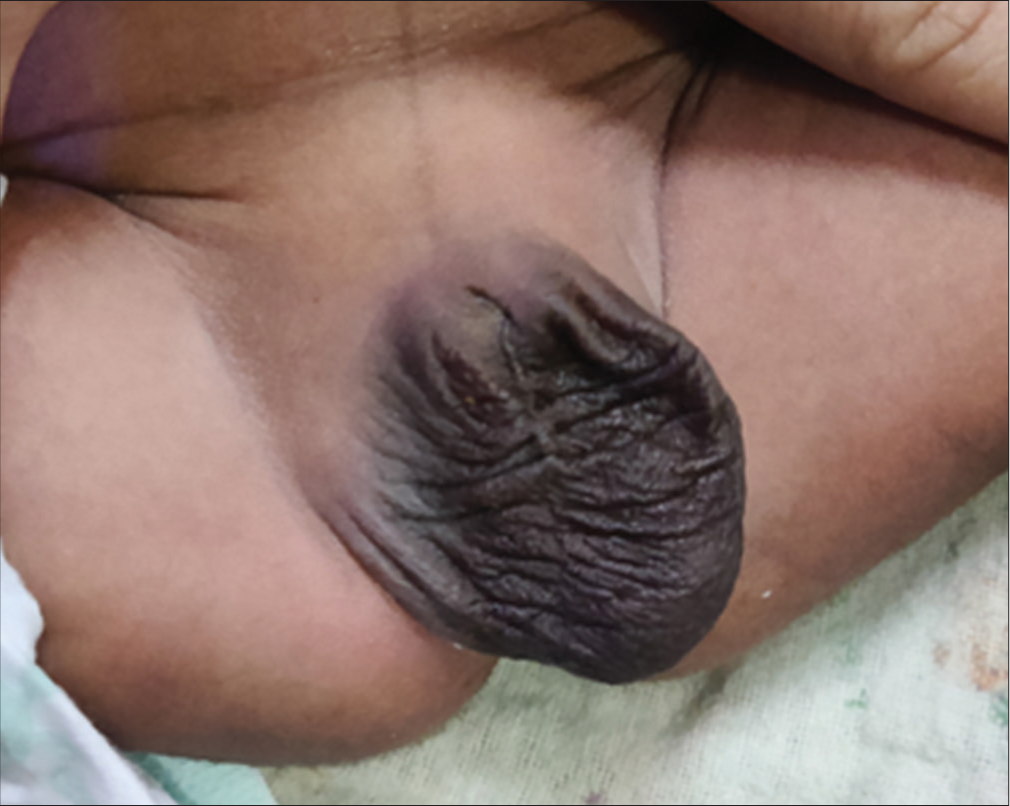
- Absent phallus with bilateral sacs with well-formed rugae with the left testis well descended and the right testis in the inguinal region.
A detailed examination of the genitals showed dribbling of urine from the urethral opening in the area of the phallus. On further examination by mechanically compressing the pre-pubic area around the phallus, with uniform pressure using the thumb, a buried penis was noted. The shaft of the penis was visible upon compression, and there was no evidence of phimosis. The stretched penile length after manual pre-pubic compression was 2.2 cm. The urethral opening was anterior. There was smegma noted with normal suprapubic fat distribution. Upon removal of the pressure, there was a retraction of the penis [Video 1].
As a part of the workup for DSD, ultrasonography confirmed bilateral testes with the right testis in the inguinal canal. There were no Mullerian structures noted. Workup for congenital adrenal hyperplasia was also normal. Fluorescence in situ hybridization analysis revealed the SRY gene and XY chromosome suggestive of a genetic male.
A diagnosis of the buried penis was made, and parents were counseled regarding the manual pre-pubic compression technique. Ultrasonography of the lower urinary tract and kidney was normal. The child was advised conservative management with a plan for definitive corrective surgery on follow-up.
Buried penis cases refer to the shaft of the penis which is abnormally fastened to the surrounding skin.[1] The causes could be the sinking of the penis under excessive suprapubic fat, tethering and shortening of the penis by abnormal fibrous bands of dartos fascia, poor penile skin fixation at the penile base, and deficient outer penile skin.[2] A manual compression test confirming a grown penis, that is protruding from the penile shaft without unbalanced retraction and sufficient penile skin is an essential step in diagnosing a buried penis. In our case, the cause of the buried penis was attributed to poor fixation at the penile base which might require corrective procedures including fixative surgeries at puberty.[3]
Ethical approval
Institutional Review Board approval is not required.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Conflicts of interest
There are no conflicts of interest.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The authors confirm that there was no use of artificial intelligence (AI)-assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
Financial support and sponsorship
Nil.
References
- Long-term outcome and parent’s satisfaction after the correction of the concealed penis. Korean J Pediatric Urol. 2009;1:58-63.
- [Google Scholar]
- Penile anomalies in adolescence. ScientificWorldJournal. 2011;11:614-23.
- [CrossRef] [PubMed] [Google Scholar]
- Commentary on “A modified fixation technique for the cure of buried penis in children”. Asian J Androl. 2023;25:144-5.
- [CrossRef] [PubMed] [Google Scholar]






